How To Apply For Medicare [Easy Step-By-Step]
Are you 65 years or older and in need of medical coverage and healthcare?
Healthcare coverage has never been more important. It can protect you and your loved ones from crippling debt and stress. Medicare is a program that can help.
Medicare is a program created by the Social Security Administration. It provides coverage for certain groups of people. Federally run Medicare has two parts, Part A and Part B.
This article will focus on Parts A and B, however, Plan C and D will be mentioned so you can understand the costs and general information of each plan. I will also cover who qualifies for Medicare, the application process, and what Medicare covers.
Quick Navigation Article Links
- Who Qualifies For Medicare
- What Does Medicare Cover
- What Costs Are Involved In Health Care Insurance
- What Is Coinsurance
- What Is Copay
- What Is Medigap
- Are Premiums And Deductibles The Same Thing
- Do I Need To Pay The Premiums For Plan A and Plan B
- How Much Are The Premiums For Plan A and Plan B
- How Much Are The Deductibles for Plan A and Plan B
- What Income Qualifies For Medicaid
- What Is Dual Eligibility and Who Pays First
- Should I Apply For Medicare Part B
- What Documents Do I Need
- What Application Do I Need To Fill Out
- How Do I Sign Up For Medicare
- What Happens After I Apply For Medicare
- How Long Does The Process Take
- How Do Check The Status Of My Application
- How Will I Know When I Am Approved And Receive Coverage
- What If I Am Rejected
- When Does My Coverage Start
Who Qualifies For Medicare
To qualify to receive Medicare you need to meet some of the following conditions:
- 65 years or older
- U.S Citizen
- A Permanent Resident who has lived in the U.S. for at least 5 years or more
- You or your spouse has paid into Medicare tax while working
- A young person with disabilities
- Someone who has End-Stage Renal Disease
What Does Medicare Cover
Medicare can cover a variety of treatments, services, tests, and prescriptions. Medicare is broken down into different parts. Each part covers specific services, tests, and supplies.
Part A is hospital insurance and Part B covers doctor’s visits and other outpatient services. Part C is called Medicare Advantage, it is another health insurance plan some individuals choose. Part D is a plan that covers prescription drugs.
What Is Part A Medicare
When you fill out your application for Medicare, the first Part you will be enrolled in is Part A. Part A covers most hospital services for the first 60 days. There are exceptions like booking a private hospital room or private nursing care.
Usually, Part A Medicare covers the following:
- Inpatient hospital visits
- Nursing facility care
- Nursing home care
- Home health care
- Hospice care
So, for example, if you have a stroke, Part A Medicare will cover your emergency hospital visit, doctor and nurses care, and rehabilitation afterward.
Make sure to talk to your doctor about your specific coverage. If you need a treatment or medical service that your Medicare doesn’t cover, you may have to pay for that treatment or service.
Use this link, https://www.medicare.gov/coverage to find out if Medicare covers your medicine, treatment, or test.
What Is Part B Medicare
Part B mainly covers Doctor and Outpatient services. Part B can include more costs. If you already have good insurance through your school or work, it may be better to stick with what you have.
Part B Medicare covers services such as:
- Clinical research
- Durable medical equipment (DME)
- Mental health (inpatient, outpatient, partial hospitalization)
- Ambulance services
- Limited outpatient prescriptions
Part B covers two different types of services. Medically necessary services or preventative services. Some preventative services may need to be paid for out of pocket but most preventative services are covered by Medicare if you receive them from a medical professional that accepts assignment.
Make sure to discuss what your plan covers with your doctor.
What Does The Term “Assignment” Mean For A Medical Professional
A medical professional who accepts “assignment” has an agreement with Medicare to agree to the payment rate they provide and to be paid directly by Medicare. A medical provider, supplier, or doctor agrees to not send you a bill for services your Medicare plan covers.
What Is Part C Medicare Advantage
Part C Medicare is private insurance that is provided as an alternative to federally run Medicare. It combines different parts of Medicare.
You need to enroll in Medicare Part A and Part B, then choose a Medicare Advantage plan and sign up for private insurance., meal services and transportation to your medical appointments can also be covered.
Part C is required to cover what federally run plans Part A and B cover. Some Medicare Advantage plans cover extra services like dental and vision care. Wheelchair ramps and shower grips.
Usually, Medicare Advantage plans are preferred provider organizations (PPOs) or health maintenance organizations (HMOs).
What are PPOs and HMOs And How Do They Work
With PPOs, you have a network of healthcare professionals and hospitals that you can visit. This option can be more flexible location-wise. However, if you visit a facility or doctor that is not listed on your plan’s network, you will probably pay more.
With HMOs, you choose or are assigned a primary care doctor. You will stay with that same doctor for all of your healthcare treatment and needs. If you need to visit a specialist or get a specific test done, your primary care doctor will refer you.
What is Part D Medicare
Part D Medicare is coverage for some of your prescription drugs. This plan must be purchased through a private insurer.
These plans usually have out-of-pocket costs, premiums, flat co-pay options, or a percentage of prescription costs. Make sure to look at the plan you are considering in detail. Ask questions when you do not understand something.
It is important to confirm that the plan will meet your budget and medical needs.
This plan has limits, if your total prescription drug costs for the year reach $4,430, you must pay 25% of your prescription costs for the rest of the year.
Visit medicare.gov to see whether the plan you are looking at will cover the medicines you need.
What Costs Are Involved In Health Care Insurance
Health care involves many different kinds of charges, fees, and payments. If you do not have insurance then you will be required to “self-pay” or pay “out of pocket” for any medical treatment you receive.
That can backfire if you become severely ill or need emergency medical care. The average hospital stay per day is about $2,873 across the United States.
Surgeries and hospital stays are VERY expensive. For example, these are the average costs of a few common surgeries:
- Heart Bypass: $123,000
- Hip Replacement: $40,364
- Heart Valve Replacement: $170,000
Imagine paying for those surgeries out of pocket!!
If you choose to buy or apply for a health care insurance plan there are still costs and fees you must pay. However, they are significantly lower than the above-mentioned costs.
Costs and fees you may have to cover with an insurance plan are:
- Premium
- Deductible
- Coinsurance
- Copayment (or “copay”)
- Services that you plan does not cover
- Prescriptions, if your plan does not cover your specific prescription
- Over-the-counter drugs, if they are not covered by your plan
It is important to read your plan carefully before you decide to purchase it. Look at the premium and deductible. See if the plan involves copay or coinsurance.
Make sure to ask the insurance rep any questions while you are reviewing the plan with them.
You can also speak to your doctor to confirm what treatments, services, and medications your plan should cover.
What Is Coinsurance
Coinsurance is a cost where you cover a percentage of your medical bills. You and your insurance provide “share” the cost of your medical bills. You may also have to cover the deductible.
For example, you could have a 75/25 plan. This means your insurance company will pay for 75% of your medical bills and you are responsible for 25% of your medical bills.
What Is Copay
Copay is a flat fee that you are responsible for paying every time you see a doctor or pick up a prescription. Copay does not count towards the deductible.
For example, say your plan has a $50.00 copayment. This means when you visit a doctor for a check-up you will pay $50.00 each time and your insurance provider will cover the rest of the cost after that.
What Is Medigap
Medigap includes different private health insurance plans that can be purchased along with Medicare in the United States.
Purchasing a Medigap policy will help you cover any medical costs that Original Medicare does not cover. Original Medicare pays for many different services, treatments, and drugs but it doesn’t cover everything. These are the “gaps” hence “Medigap”.
Medicare does not cover your Medigap policy, you must purchase this separately. A Medigap policy is not the same as a Medicare Advantage policy.
Medigap must meet the strict standards of Federal and State laws, this is to protect you, the customer.
What Medigap Covers
Please see the chart below to understand what each Medigap policy covers:
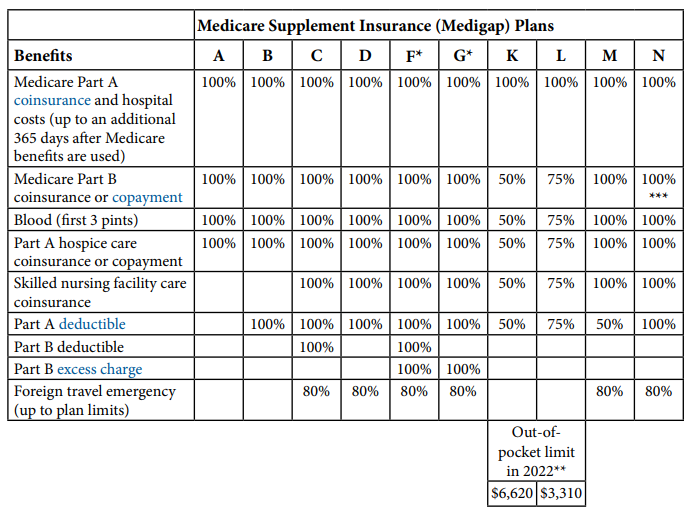
Medigap plans do not cover long-term care, vision, hearing aids, dental care, glasses, or private nursing.
Medigap does not include Medicare Part C plans, Medicare Part D plans, or Medicaid. Tricare, Veterans Benefits, and employer or union health care plans are not covered. Long-term insurance policies, Indian Health Service, Tribal Health Service, or Urban Indian Health Plans are not covered. Lastly, Qualified Health Plans that are sold by Health Insurance Marketplace are not covered in Medigap.
Companies that sell Medigap policies do not have to offer you every Medigap plan. They can offer you specific policies or a “standardized” Medigap policy.
If they offer you any Medigap policy they must also offer you Plan A. If they offer other add-on plans besides Plan A they must also offer you Plan C or Plan F. (See chart above)
Read more about the plans Medigap offers, their coverage, and what qualifies you by clicking this link.
Are Premiums And Deductibles The Same Thing
The “premium” is the amount that you pay on a regular basis to your insurance company. Premiums can be paid monthly, bi-yearly, or yearly. The premium amount and billing frequency will be based on the insurance plan you choose and the company that provides that plan.
You must continue to pay your premium even if you do not use the plan or have an emergency. If you stop paying your premium, you will no longer be covered for any medical costs.
The “deductible” is the fee or amount that you must pay before your insurance kicks in and covers the rest of the bill.
For example, if your deductible is $1000, this means if you go to the hospital for an emergency, when you pay your bill you need to pay $1000 and your insurance plan will cover the rest.
You can choose a higher or lower deductible for your plan, but a lower deductible may increase your monthly premium payments.
Do I Need To Pay The Premiums For Plan A and Plan B
You qualify for Part A Medicare Coverage without having to pay premiums if you are age 65 and:
- You receive Railroad Retirement Board or Social Security Retirement Benefits.
- You qualify to receive Railroad Retirement Board or Social Security Retirement Benefits but have not yet filed for either of them.
- You or your spouse had employment with Medicare-covered benefits.
If you or your mate are 65 years or older, US citizens or permanent residents, and did not pay any Medicare taxes which you were working, you may be able to purchase Medicare Part A.
If you are someone under 65 years of age, you could qualify for Medicare Part A without having to cover any premiums if:
- You have worked long enough to be eligible for Railroad Retirement Board or Social Security Retirement Benefits for 24 months.
- You have received a kidney transplant or are a kidney dialysis patient.
- You have Lou Gehrig’s disease.
You can use this link Medicare.gov eligibility tool to see if you are eligible for Medicare and what your premium would be.
However, Medicare Part B premiums must be paid. The premium for Part B is taken from your Social Security, Civil Service Retirement, or Railroad Retirement check each month.
How Much Are The Premiums For Plan A and Plan B
For Medicare Part A if you worked for at least 10 years and paid Medicare taxes, you don’t need to pay any premiums.
Each year that you work and pay into Social Security or Medicare, you receive quarters or credits. If you work 10 years you would have 40 quarters.
If you have 30-39 quarters you would pay a premium of $226.00 for Part A. And if you have less than 30 quarters, the premium you pay would be $411.00
If you signed up for Part B before 2016 your premium should be around $104.90 each month.
If you enrolled in Part B in 2016, your deductible would be $121.80. If you arent receiving Social Security payments yet or are billed directly for your Plan B coverage, your premium would generally be $121.80.
If you worked for the railroad, you need to contact the Railroad Retirement Board to understand more about your Plan B premium costs.
The premium can be higher if you make more than $88,000 annually. The government will review your tax returns and calculate your premium.
The table below shows how your premium may be calculated:
How Much Are The Deductibles for Plan A and Plan B
The deductible for Part A in 2023 is $1,600.00. There are certain supplemental plans you can purchase to cover the deductible and certain out-of-pocket payments. Medigap is one such service.
The deductible for Plan B in 2023 is $226. With Part B you will also be responsible for covering 20% of all doctors visits and other outpatient services you receive.
What Income Qualifies For Medicaid
If you are disabled or make below a certain amount each year you could qualify for Medicaid. This is a jointly run assistance program. It is provided by both the federal government and individual states.
The income that qualifies you for Medicaid is different in each state. To find out if you qualify you will need to contact Medicaid, a licensed insurance agency, or Medicare.
Certain plans that are offered can save you money, to learn more you need to contact Medicare plan directly or call Medicare at 1-800-MEDICARE (1-800-633-4227). The number 1-877-486-2048 can be used by TTY users.
You could also contact a licensed insurance agency like Medicare Consumer Guide’s company eHealth. The number to contact eHealth is 888-391-2659
Please visit this like to check if your income qualifies and learn your specific state’s criteria.
You can call your State Medical Assistance (Medicaid) office to learn more and confirm that you qualify.
In some states, if your income is too high to qualify for Medicaid you can “spenddown” to lower your income.
What Is Spenddown
Spenddown is a method of lowering your income by subtracting all medical expenses from your income. If you do this you may be able to qualify for Medicaid because you could be classified as “medically needy”.
What Is Dual Eligibility and Who Pays First
If you qualify for both Medicare and Medicaid then you can use both provisions. Most of your medical expenses should be covered.
Medicare will pay all your medical bills first and if there is anything Medicare does not cover Medicaid then pays.
Medicaid will never pay first for any services or treatments that are covered by Medicare.
Should I Apply For Medicare Part B
When applying online, you can apply for Part A and Part B at the same time. You must pay a premium to receive Part B coverage. You have the option to turn down Part B.
If you turn down applying for Part B, if you want it later, your coverage may be delayed for a while. You may also have a higher premium.
The premium you would pay for delayed Part B coverage goes up by 10% every 12 month period where you are eligible for Part B but choose not to have it.
However, if you qualify for the Special Enrollment Period (SEP) your premium may not be increased if you initially opt out of Part B.
What Is The Special Enrollment Period
The Special Enrollment Period allows you to enroll for Part B later if you have an insurance plan under your or your spouse’s employment. You may qualify for the Special Enrollment Period under two conditions.
They are:
- You apply for Part B during any month that you or your spouse’s employment continues or you remain covered with a group health plan.
- You apply for Part B during the 8-month period that starts after the group health plan or your employment that provides the plan ends.
What Documents and Information Do I Need To Provide
You can sign up for Medicare at the same time you apply for your Social Security Benefits. However, if you have not done that, you will need to apply for Medicare only.
When applying for Medicare only you need to provide the following documents:
- Birth Certificate to prove date and place of birth if you have a different name now.
- Proof of US citizenship.
- If you are a permanent resident you need to provide a Permanent Residency Card.
- Medicaid number
- Current Health Insurance information, start and end date, policy, insurance companies name, employers name that provides the insurance.
Look over this document to confirm the documentation you will need.
What Application Do I Need To Fill Out
If you are eligible for applying for Social Security retirement benefits you should automatically be eligible for Medicare Part A. Applying for Part A should be included in the Retirement Benefits Application.
To apply for Medicare Part B you need to fill out the CMS 40B Application For Enrollment in Medicare Part B (Medical Insurance).
If you are applying for Medicare because you have a low income you need to fill out the SSA-44 Medicare Income-Related Monthly Adjustment Amount – Life-Changing Event
How Do I Sign Up For Medicare
You should be able to sign up for Medicare three months before you turn 65. Some people are automatically eligible to receive Medicare coverage.
You can sign up at your local Social Security office In-Person.
You can also sign up online at the SSA website. This method is the fastest and easiest way to sign up for your coverage. You need to log into your my Social Security account and fill out the application for Part A Medicare.
You can also sign up over the phone by calling Social Security at 1-800-772-1213. The number 1-800-325-0778 can be used for TTY users.
If you or your partner were employed by a railroad, you need to call the Railroad Retirement Board at their number 1-877-772-5772.
Avoid Phone Scammers
Please be careful when taking ANY phone call about your Social Security benefits!!! Unfortunately, there are quite a few scams related to Social Security numbers. A Social Security officer will NEVER threaten you or say you will go to jail if you do not give them your personal information.
If you receive a phone call where someone says “there is a charge against you, you will go to jail if you do not pay money or give us your information” that is a scam! Hang up!
What Happens After I Apply For Medicare
Once you have completed and submitted your application the Centers for Medicare and Medicaid Services (CMS) will send you a Welcome To Medicare packet. This should be mailed to your home address.
You will also get a Medicare and You book that included important information in your coverage choices.
How Long Does The Process Take
If you apply online for your benefits and Medicare the application process should take no longer than 60 minutes.
Make sure to have all your information and documents on hand. If you need to pause and come back to the application later, just save the application.
Once you have submitted your application you will receive your Welcome To Medicare packet. This could take 6-12 weeks.
If you do not hear anything from Social Security or Medicare you can call your local office to speak to an agent about your application.
How Do Check The Status Of My Application
You can view your application status for Medicare or Medicaid online. Log into your my Social Security account and look for the application status tab.
You can check your application status by visiting MyMedicare.org and view the “Check Enrollment” page.
You can also find the status of your application by calling your local social security office and asking an agent.
How Will I Know When I Am Approved And Recieve Coverage
Once your application is processed, reviewed, and approved you should receive an acceptance letter 45 to 90 days after you submitted your application.
This letter will come with a Welcome To Medicare packet that gives more information and details on how to use your plan. The package should include your Medicare card.
You may also receive a reminder letter 1 month before your Medicare coverage becomes active.
View a sample here.
What If I Am Rejected
If you are rejected for Medicare or Medicaid you can call your local Social Security office to learn more and confirm you provided the correct information.
If you were denied because you did not provide the correct information then you need to reapply and give the correct document.
If you were rejected because you were deemed not eligible you may have to wait until you become eligible. If you believe you are eligible, you need to request
When Does My Coverage Start
The way you apply and when you apply will affect when your coverage begins. Your coverage may start immediately or 3 months after you apply.
Once your coverage starts, you will not need to reapply each year.
You can make a change or adjust your plan during the open enrollment period. This is from October 15th to December 7th of each year.
